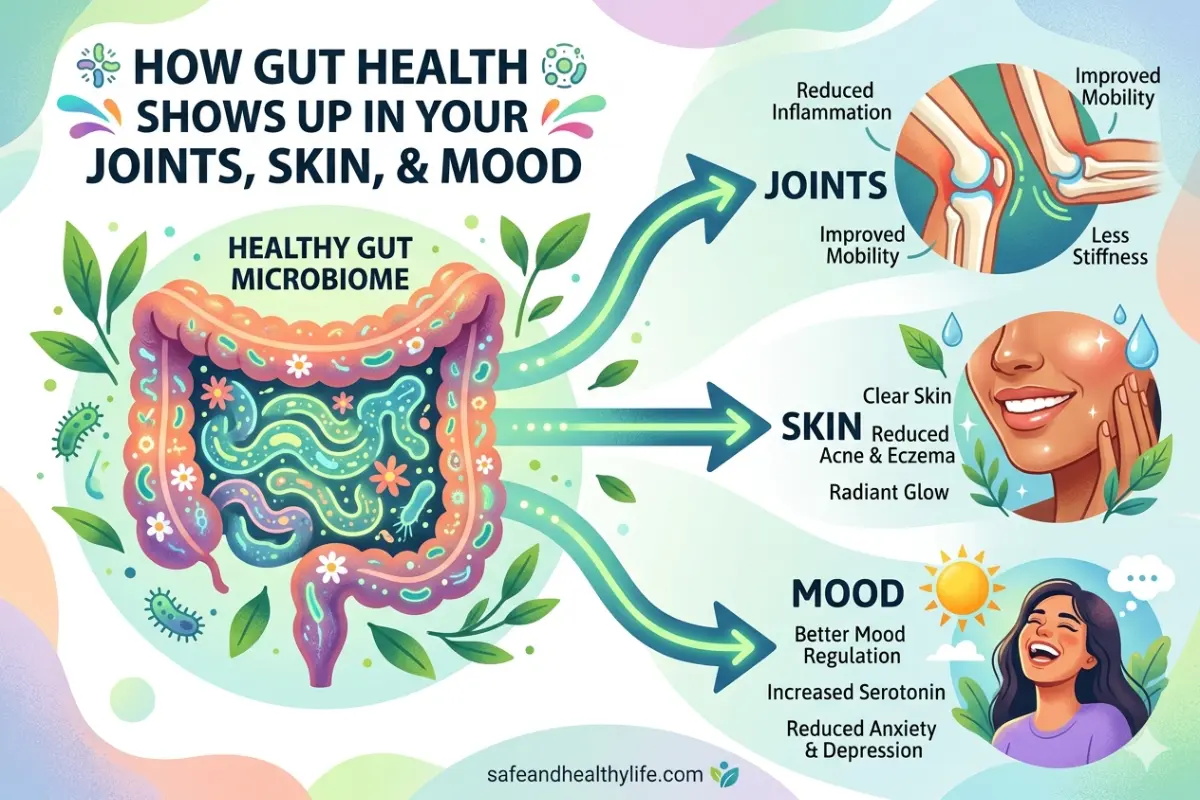
TL;DR: Silent inflammation is a low-grade process that affects how you feel long before a medical diagnosis. The gut is a central regulator of this process. It affects areas that seem unrelated at first glance. This article explains how gut health shows up in your joints, skin, and mood. You’ll learn how supporting your gut can restore internal harmony.
Inflammation is often associated with visible swelling or acute injury, yet some of the most disruptive inflammatory processes happen quietly over time. This type of low-grade inflammation can affect how the body feels and functions long before a clear diagnosis is made. Many people notice subtle symptoms like ongoing joint stiffness, recurring skin issues, or persistent mood changes without realizing these experiences may share a common origin.
In recent years, growing attention has been placed on the gut as a central regulator of overall health. The digestive system does far more than process food. It plays a key role in immune balance, hormone signaling, and communication with the brain. When gut health is compromised, the effects can ripple outward, showing up in areas that may seem unrelated at first glance.
How does the gut act as the body’s immune gatekeeper?
The gut acts as an immune gatekeeper by housing most of the immune system and forming a barrier against the outside world. It lets nutrients pass but keeps harmful substances out. When this barrier fails, inflammatory signals ripple through the body. This affects tissues far beyond the digestive tract.
The gut houses a large portion of the immune system, acting as a frontline barrier between the body and the outside world. The lining of the digestive tract is designed to allow nutrients to pass through while keeping harmful substances at bay. When this balance is maintained, immune activity remains regulated, and inflammation stays within a healthy range.
Problems arise when the gut barrier becomes less effective. At that point, inflammatory signals can increase, prompting immune responses that do not resolve properly. This process does not always cause digestive discomfort. Instead, it may quietly influence tissues throughout the body.
A common question that arises for people learning about this connection is “What is leaky gut?” The term refers to increased intestinal permeability, where gaps in the gut lining allow particles to enter circulation that would normally stay contained. This can trigger ongoing immune activation that contributes to silent inflammation rather than an immediate illness.
Can gut imbalance affect joint health?
Yes, gut imbalance can directly affect joint health. When the gut is out of balance, inflammatory compounds can enter the bloodstream. These compounds can settle in joint tissues, leading to ongoing stiffness, soreness, and reduced mobility. This process is a classic sign of how gut health shows up in your joints.
Joint discomfort is often attributed to aging, overuse, or mechanical wear. While these factors matter, inflammation driven by gut imbalance can also play a role. Inflammatory compounds circulating in the bloodstream can settle in joint tissues, leading to stiffness, soreness, or reduced mobility over time.
This type of discomfort may feel unpredictable. Symptoms may flare and subside without clear physical triggers. Some people notice joint issues that migrate between areas rather than staying localized. These patterns can reflect systemic inflammation rather than isolated joint damage.
Supporting gut health may help modulate these inflammatory signals. Balanced digestion, diverse gut bacteria, and a resilient gut lining all contribute to calmer immune responses that reduce the burden placed on joints and connective tissue.
A 2025 review published in Frontiers in Immunology highlights that specific gut microbes, such as Lactobacillus and Bifidobacterium, can help preserve the intestinal barrier and slow the progression of joint inflammation in conditions like rheumatoid arthritis.
Why is the skin considered a visible signal of internal health?
The skin is considered a window into internal balance because it is a barrier system closely connected to the gut. When the gut triggers systemic inflammation, the skin may respond with its own inflammation. This can show up as pervasive dryness, redness, sensitivity, or breakouts.
The skin is often considered a window into internal balance. Conditions like persistent dryness, redness, breakouts, or sensitivity can sometimes indicate more than surface-level problems. Because the skin and gut are both barrier systems, they are closely connected through immune and inflammatory pathways.
When the gut triggers ongoing immune activity, the skin may respond with inflammation of its own. This can disrupt oil production, weaken the skin barrier, or increase reactivity to environmental factors. While topical treatments can help manage symptoms, they may not address underlying drivers.
Improving gut function can support skin health by reducing inflammatory signals at their source. Over time, this internal support may lead to improvements in texture, tone, and resilience that external products alone may not deliver.
Emerging research from 2025 emphasizes that “intestinal dysbiosis“, an imbalance in gut bacteria, is a root cause of systemic inflammation that directly impairs skin homeostasis, potentially leading to conditions like psoriasis and acne.
Is there a link between mood, brain chemistry, and the gut connection?
Yes, there is a powerful link. The gut and brain constantly communicate. Many neurotransmitters that regulate mood are influenced by gut activity. Inflammation that starts in the digestive system can alter these signaling pathways, contributing to low mood, irritability, and mental fatigue.
Mood changes are frequently attributed to stress, life circumstances, or chemical imbalances in the brain. While these factors are real, they do not exist in isolation. The gut and brain are in constant communication through neural pathways, immune responses, and chemical messengers.
A significant portion of neurotransmitters involved in mood regulation are influenced by gut activity. When inflammation originates in the digestive system, it can alter these signaling pathways. This can contribute to feelings of low mood, irritability, or mental fatigue that lack a clear external cause.
Chronic inflammation may also affect how the body responds to stress. Individuals may feel less resilient or experience longer recovery times after emotional challenges. Supporting gut health can help stabilize these systems, promoting more consistent energy and emotional balance.
New clinical insights from 2025 and 2026 suggest that “psychobiotics” (specific probiotics for mental health) can influence the production of mood-regulating neurotransmitters like serotonin and GABA, offering new ways to manage anxiety and depression.
Reducing Silent Inflammation Through Gut Support

Addressing silent inflammation involves looking beyond symptoms and focusing on foundational health. Supporting the gut starts with habits that promote balance rather than quick fixes. Regular meals with whole foods, sufficient fiber, and hydration help nourish beneficial bacteria.
Stress management also plays a role. Prolonged stress can alter gut function and exacerbate inflammatory responses. Incorporating restorative practices such as mindful movement, adequate sleep, and regular downtime supports both digestive and immune balance.
Gentle consistency matters more than extreme measures. Gradual improvements in gut support often lead to more sustainable changes throughout the body. Over time, reduced inflammatory pressure can ease joint discomfort, support clearer skin, and contribute to more stable mood patterns.
Conclusion
Silent inflammation can quietly influence how the body feels and functions, often showing up in unexpected ways. The gut plays a central role in regulating immune responses that affect joints, skin, and mood. By understanding this connection and supporting digestive health, it becomes possible to address inflammation at its source. A balanced gut can help restore internal harmony, allowing the body to respond more calmly and resiliently over time.
Frequently Asked Questions
1. Can bad gut health make your joints hurt?
Your gut and your joints are connected by inflammation. An unhealthy gut can lead to systemic inflammation. That can affect your joints, causing stiffness and soreness. This is how gut health shows up in your joints.
2. Can leaky gut cause mood swings?
The gut and brain constantly communicate. A compromised gut barrier can cause systemic inflammation. This can alter neurotransmitter signaling, which can contribute to low mood and irritability.
3. Does supporting gut health help skin?
Improving gut function can reduce inflammatory signals at their source. This can lead to calmer skin with better texture and resilience. Internal support often delivers results that external products alone may not.
4. How can I lower inflammation in my gut?
Focus on foundational habits, not quick fixes. Eat whole foods, get sufficient fiber, and stay hydrated. Also, managing stress is vital for lower gut inflammation.
Not always, but there is often a powerful gut connection. When multiple subtle symptoms appear together, it may indicate that they share a common origin in gut health. This is a subtle way that gut health shows up in your joints, skin, and mood.
About The Author:
Elena Swan is a freelance health and wellness writer specializing in mental illness. She likes researching complex health topics and presenting the information in a way that everyday people can understand so they can apply it to their own lives. View her portfolio at elenaswanwrites.com.




