
TL;DR: Nearly 75% of Americans report physical or emotional symptoms of stress, according to the APA. This guide covers everything you need to manage it: what stress does to your body, 5 fast-relief techniques, the food-stress connection, how sleep and exercise help, teen and burnout stress, and when to get professional help. Every section links to a deeper dive so you can go as far as you need. Read it all, or jump straight to the part that hurts most right now.
We’ve all been there. Your heart is pounding, your jaw is clenched, and your brain is running in seventeen directions at once. You can’t focus. You can’t sleep. And no matter how many times you tell yourself to calm down, nothing shifts.
You’re not alone in this. Nearly 75% of Americans report physical or emotional symptoms caused by stress, according to the American Psychological Association. And 49% of Americans say they experience significant daily stress, making the US one of the most stressed nations in the developed world.
Stress management isn’t about eliminating stress from your life. That’s not possible, and honestly, some stress is useful. It’s about learning how to work with your body’s response instead of being hijacked by it.
That’s exactly what this guide is built for. Whether you’re dealing with work pressure, family demands, health anxiety, or just that low-level hum of overwhelm that never quite goes away, you’ll find practical, research-backed answers here. We’ve covered every angle so you can start where it hurts most.
Table of Contents
- What Is Stress, and Why Does Your Body React That Way?
- What Are the Most Common Signs of Stress?
- 5 Quick Stress Relief Techniques You Can Use Right Now
- How Exercise Lowers Stress (and Which Types Work Best)
- What Should You Eat (and Avoid) When You’re Stressed?
- How Stress Wrecks Your Sleep (and How to Break the Cycle)
- Mindfulness and Meditation: Do They Actually Work?
- Stress in Teenagers: Signs Parents Should Know
- What Is Burnout, and How Is It Different from Stress?
- Long-Term Stress Management: Building a Daily Routine That Sticks
- When Should You Seek Professional Help for Stress?
- Your Complete Stress Management Resource Directory
- Frequently Asked Questions
What Is Stress, and Why Does Your Body React That Way?
Stress is your body’s natural response to demands it perceives as threatening or overwhelming. When triggered, your brain releases cortisol and adrenaline, raising your heart rate and blood pressure. This “fight or flight” response is helpful in short bursts but damages your health when it stays switched on for weeks or months.
Here’s what’s actually happening inside you. Your hypothalamus (a small region deep in the brain) acts like an alarm system. The moment it senses a threat, it signals your adrenal glands to pump out adrenaline and cortisol. Your heart speeds up. Your breathing gets shallow. Your muscles tense, ready for action.
Think of it like your car alarm going off when there’s no burglar. The system works exactly as designed. The problem is when it never gets a chance to switch off.
There’s an important difference between the two types of stress you should know:
Acute stress is short-term. A work deadline, a difficult conversation, a near-miss on the highway. It comes on fast and fades when the situation passes. In small doses, this kind of stress can actually sharpen your focus and improve performance.
Chronic stress is the dangerous kind. It’s the stress that never fully resolves. Week after week, your body stays in a low-level state of alarm. Gallup research shows that 49% of Americans experience this kind of significant daily stress, with cortisol levels staying elevated far longer than they should.
Over time, chronically elevated cortisol suppresses your immune system, disrupts your sleep, raises blood pressure, and contributes to weight gain, particularly around the abdomen. It’s not just uncomfortable. It’s genuinely harmful.
Want to know exactly how this plays out in your body? Read our detailed breakdown of what chronic stress does to your body to see the full picture.
What Are the Most Common Signs of Stress?
The most common signs of stress include headaches, trouble sleeping, irritability, muscle tension, fatigue, and difficulty concentrating. Emotionally, stress can feel like constant worry, low mood, or a sense of being out of control. Many people don’t realize stress is the cause until symptoms become persistent and begin affecting daily life.
It’s worth separating the signs into two categories, because stress often disguises itself.
Physical signs of stress:
- Headaches or migraines that come and go
- Muscle tension, especially in the neck, shoulders, and jaw
- Digestive issues like stomachaches, nausea, or IBS flare-ups
- Fatigue that doesn’t improve with sleep
- Frequent illness (your immune system takes a hit)
- Chest tightness or a racing heart
- Skin breakouts or flare-ups of eczema or psoriasis
Emotional and behavioral signs of stress:
- Irritability or a short temper that feels out of proportion
- Difficulty concentrating or making decisions
- Constant low-level worry that won’t switch off
- Withdrawing from people or activities you normally enjoy
- Over-eating or under-eating in response to how you feel
- Reaching for alcohol, caffeine, or screens to cope
One thing worth noting: stress and anxiety can look almost identical from the outside. The key difference is that stress usually has an identifiable trigger. Something is causing it. Anxiety often lingers even when there’s nothing specific to point to. Both are manageable, but they may need different approaches.
If you’ve been noticing several of these signs consistently for more than a couple of weeks, it’s worth taking them seriously. Check out our full guide on the emotional signs of stress and what they mean for your mental health.
5 Quick Stress Relief Techniques You Can Use Right Now
The five most effective quick stress relief techniques are box breathing (4 counts in, hold, out, hold), the 5-4-3-2-1 grounding method, progressive muscle relaxation, cold water on your wrists or face, and a 5-minute outdoor walk. Each activates the body’s parasympathetic nervous system, lowering cortisol and slowing your heart rate within minutes.
These aren’t just feel-good suggestions. Stanford Medicine research shows that just 5 minutes of intentional breathing exercises each day measurably reduces overall anxiety and improves mood. Your nervous system responds to breath signals faster than almost anything else.
Here’s how to use each one:
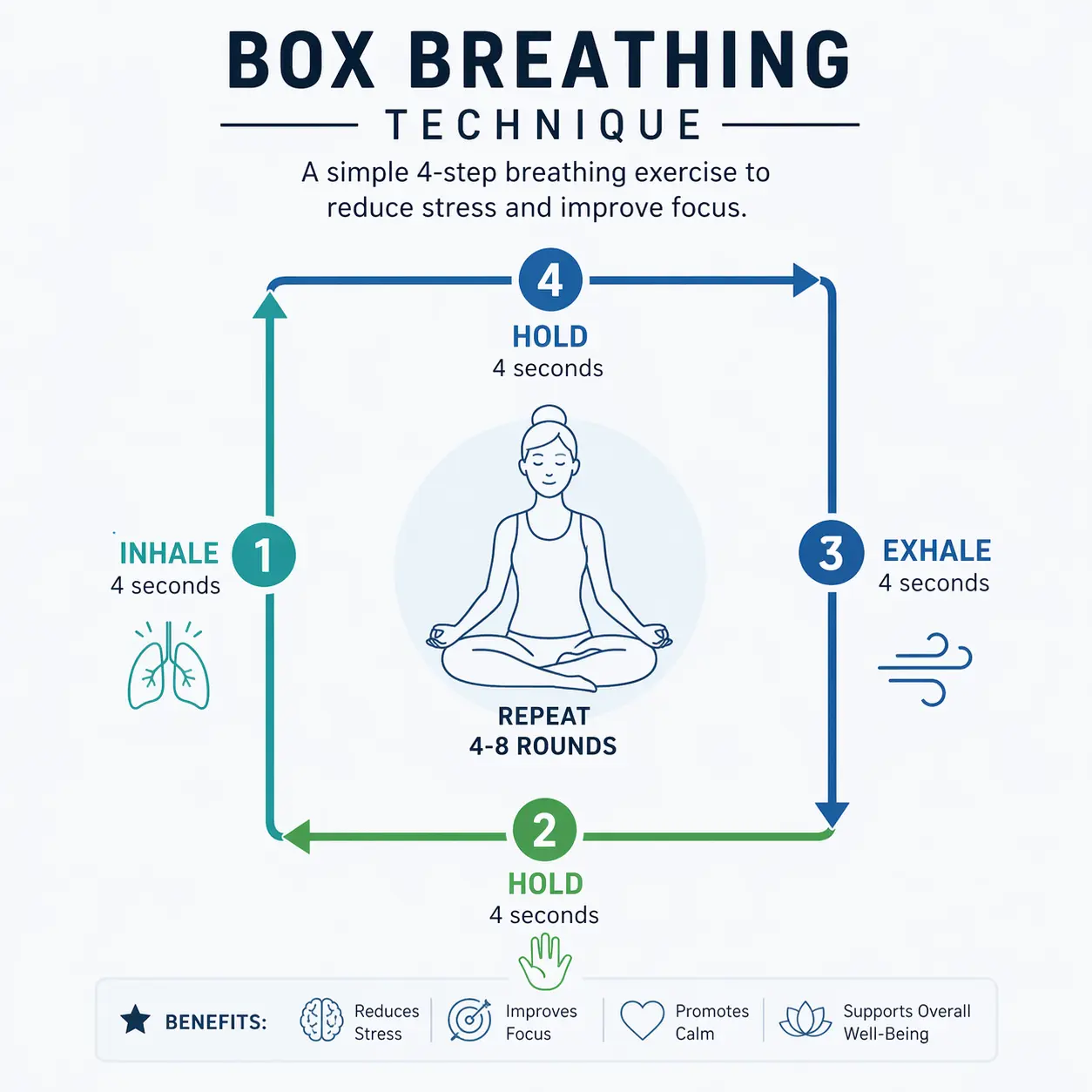
1. Box Breathing (4-4-4-4)
Inhale slowly for 4 counts. Hold for 4 counts. Exhale for 4 counts. Hold for 4 counts. Repeat 4 times. Navy SEALs use this technique to stay calm under extreme pressure. If it works in combat, it’ll work in your kitchen at 11 pm.
2. The 5-4-3-2-1 Grounding Method
Name 5 things you can see. 4 things you can touch. 3 things you can hear. 2 things you can smell. 1 thing you can taste. This technique yanks your brain out of the spiral and into the present moment. It’s particularly effective during moments of sudden overwhelm or panic.
3. Progressive Muscle Relaxation
Start at your feet. Tense each muscle group tightly for 5 seconds, then release completely. Work your way up your body: calves, thighs, stomach, chest, hands, arms, shoulders, face. By the time you reach the top, your body feels noticeably lighter. Most people fall asleep doing this at night.
4. Cold Water on Your Wrists or Face
Splashing cold water on your face or running it over your wrists triggers the “dive reflex,” which slows your heart rate rapidly. It sounds too simple to work. It isn’t. Keep this one in your back pocket for when you need something fast.
5. A 5-Minute Walk Outside
Even a short outdoor walk lowers cortisol levels measurably. Add natural light and you also get a serotonin boost. You don’t need a park or a trail. A lap around your block works perfectly.
I started combining techniques 1 and 5 about two years ago, a quick breathing cycle before stepping outside. The difference in how I processed the rest of the day was noticeable within the first week. Nothing dramatic. Just less reactive, more grounded.
Want more techniques like these? We’ve got a full list in our post on more quick stress relief techniques that you can start using today.
How Exercise Lowers Stress (and Which Types Work Best)
Here’s something most people know but underestimate: exercise is one of the most powerful stress-reduction tools your body has. And it doesn’t require an hour at the gym.
When you move your body, two things happen. First, cortisol levels drop. Second, your brain releases endorphins, the natural chemicals that create a sense of calm and well-being. This isn’t motivational language. It’s basic physiology.
The American Psychological Association recommends at least 150 minutes of moderate physical activity per week for measurable mental health benefits. That breaks down to roughly 20–30 minutes on most days. Very manageable.
The best types of exercise for stress relief, in order of research support:
1. Moderate aerobic exercise (walking, swimming, cycling, light jogging) is the most consistently effective for lowering cortisol. A 20-minute walk in daylight is enough to shift your stress response within the hour.
2. Yoga combines movement, breathwork, and mindfulness into one practice. Multiple studies show it reduces both cortisol levels and perceived stress better than rest alone.
3. Strength training at a moderate intensity releases endorphins and improves sleep quality, both of which directly support stress resilience over time.
One important caveat: intense daily exercise (high-volume HIIT every single day, for example) can actually spike cortisol rather than lower it. More isn’t always better. Consistency at a moderate level beats intensity.
You don’t need equipment or a gym membership to get started. Our collection of stress-relieving home workouts has everything you need to begin today. And if you’re looking to build movement into your mornings, our guide to daily exercise for stress relief shows you exactly how to make it stick.
What Should You Eat (and Avoid) When You’re Stressed?
Foods that help lower stress include magnesium-rich options like dark leafy greens, pumpkin seeds, and dark chocolate, plus omega-3 fatty acids from salmon and walnuts. Avoid caffeine, alcohol, and ultra-processed foods when stressed. They raise cortisol and disrupt the gut-brain axis, making stress harder to manage over time.
There’s a reason your gut is called your “second brain.” The gut-brain axis is a two-way communication system between your digestive tract and your central nervous system. When stress disrupts your gut, your mood and mental clarity suffer. And when your diet is poor, your stress response gets worse. It runs in both directions.
Here’s a simple split to work with:
Eat more of:
- Magnesium-rich foods: dark leafy greens (spinach, kale), pumpkin seeds, dark chocolate (70%+), avocado, black beans
- Omega-3 fatty acids: salmon, sardines, walnuts, flaxseeds
- Probiotic foods: yogurt, kefir, kimchi, sauerkraut (supporting gut health supports mood)
- Complex carbohydrates: oats, sweet potatoes, brown rice (help stabilize blood sugar and serotonin)
Cut back on:
- Caffeine after noon (it keeps cortisol elevated and disrupts sleep)
- Alcohol (it feels calming, but disrupts sleep architecture and raises anxiety the next day)
- Ultra-processed foods and refined sugar (they spike and crash blood sugar, amplifying stress)
Here’s a fact most people don’t expect: being just half a liter dehydrated can raise your cortisol levels noticeably. Research has shown that even mild dehydration triggers a measurable stress response. Before you reach for anything else, drink a glass of water.
The stress-eating cycle is real, and it’s worth addressing directly. When you’re stressed, your body craves high-fat, high-sugar foods because cortisol drives these cravings. Eating them provides short-term comfort but leaves you more depleted. Breaking the cycle starts with noticing the urge before acting on it; even a 10-second pause helps.
Building a diet that genuinely supports your stress response starts with getting more of the right foods in daily. Our guide on greens that support stress relief is a great place to start.
How Stress Wrecks Your Sleep (and How to Break the Cycle)
Stress disrupts sleep by keeping cortisol elevated at night, making it hard for the brain to wind down. Poor sleep then raises cortisol further the next day, creating a damaging loop. Breaking this cycle requires consistent sleep timing, a pre-bed wind-down routine, and addressing the stress source directly, not just the insomnia.
This is one of the most frustrating patterns in stress management. You’re exhausted, but you can’t sleep. And because you can’t sleep, tomorrow’s stress feels even harder to handle. Then the cycle repeats.
The APA’s annual poll found that 53% of adults say stress is the single biggest factor affecting their mental health, with sleep problems following close behind. The two are deeply linked, and you can’t fully fix one without addressing the other.
Here’s why it happens. Cortisol is designed to peak in the morning (to wake you up) and decline gradually through the day, reaching its lowest point at night. Chronic stress disrupts this curve, keeping cortisol elevated at times it should be low. Your brain gets the signal to stay alert when it should be winding down.
Three things that break this cycle:
1. Lock in a consistent sleep and wake time. Your body clock (circadian rhythm) runs on regularity. Going to bed and waking up at the same time every day, even on weekends, is the single most effective sleep intervention. The CDC recommends 7–9 hours per night for adults for optimal mental and physical health.
2. Build a wind-down routine. Start 30–45 minutes before bed. No screens (the blue light suppresses melatonin). Something low-stimulation: light stretching, reading a physical book, a warm shower, or a few minutes of journaling. The routine itself trains your nervous system that sleep is coming.
3. Write it down before you lie down. One of the most common reasons people can’t fall asleep is that their brain is processing unfinished thoughts. Spend 5 minutes before bed writing down tomorrow’s tasks and any worries on your mind. It’s called a “cognitive offload,” and it works by giving your brain permission to let go.
Want to understand exactly why your brain won’t stop running at night? Our post on why stress keeps your brain awake breaks it down clearly.
Mindfulness and Meditation: Do They Actually Work?
Yes, and the evidence is strong. Mindfulness meditation is one of the most thoroughly researched stress management tools we have. Harvard Medical School research shows that a consistent mindfulness practice can reduce cortisol by up to 25% over 8 weeks, improve sleep quality, and build emotional resilience. Even 5–10 minutes of daily practice produces measurable changes in how the brain responds to stress.
Mindfulness, in the plainest terms, is paying attention to the present moment without judging what you find there. That’s it. You’re not trying to empty your mind. You’re just noticing what’s happening, your breath, your body, your surroundings, without immediately reacting to it.
There are two ways to practice:
Formal meditation means setting aside time to sit quietly and focus on your breath or a guided audio. Apps like Insight Timer (free), Calm, and Headspace make this accessible even if you’ve never meditated before.
Informal mindfulness means bringing that same quality of attention into everyday activities. Mindful eating means actually tasting your food instead of scrolling. A mindful walk means noticing what’s around you instead of running through tomorrow’s to-do list. These moments add up.
The Mayo Clinic confirms that regular meditation can help manage stress-related conditions, including anxiety, depression, high blood pressure, and chronic pain. It doesn’t replace treatment for serious conditions, but it’s a powerful complement to it.
For those dealing with anxiety alongside stress, mindfulness-based cognitive therapy (MBCT) is worth researching. It’s a structured program combining meditation with cognitive behavioral techniques, and it has a strong track record for reducing anxiety relapse.
If you’re finding that stress is tipping into something that feels bigger than what mindfulness can hold, our guide on professional support for stress explains the options clearly.
Stress in Teenagers: Signs Parents Should Know
Teen stress is rising sharply, and it looks different from adult stress. The APA’s most recent data shows that nearly two-thirds of younger adults feel weighed down by national-level stressors, with Gen Z reporting the highest stress levels of any age group. For teenagers specifically, the top triggers are academic pressure, social media, social comparison, and uncertainty about the future.
The tricky part for parents is that stressed teenagers often don’t say “I’m stressed.” They show it in other ways.
Signs to watch for:
- Changes in sleep patterns (sleeping significantly more or less than usual)
- Increased irritability or emotional outbursts that feel out of proportion
- Withdrawing from family, friends, or activities they used to enjoy
- Declining grades or difficulty concentrating at school
- Physical complaints without a clear medical cause (headaches, stomachaches)
- Changes in eating habits
If you’re seeing several of these consistently, here are three things that actually help:
Open the conversation without pressure. Don’t lead with “what’s wrong?” Try “You seem like you’ve got a lot going on. I’m here if you want to talk.” Low-pressure, no agenda. Teens shut down when they feel interrogated.
Reduce outcome-based pressure. A lot of teen stress is driven by the fear of failing or disappointing people. Shifting the conversation from results to effort (“I’m proud of how hard you worked on that”) reduces the pressure significantly over time.
Encourage physical outlets. Movement, sports, creative activities, and time with friends in real life (not on screens) are the most effective natural stress regulators for teenagers. Help them protect time for these.
For a full breakdown of what to watch for, our post on stress signs in teenagers is worth reading. And if you’re looking for practical conversation strategies, our guide on helping your teen cope with pressure gives you the specific language to use.
What Is Burnout, and How Is It Different from Stress?
Burnout is a state of chronic physical and emotional exhaustion caused by prolonged, unrelieved stress, most often from work or caregiving. Unlike regular stress, which feels urgent and overwhelming, burnout feels empty and detached. Recovery takes weeks or months, not days, and usually requires structural changes alongside personal coping strategies.

This distinction matters. If you try to treat burnout with the same techniques you’d use for acute stress (a weekend away, a good night’s sleep, a meditation session), you’ll be frustrated when they don’t work. Burnout is a different animal.
Here’s how the stages typically progress:
Stage 1: Stress. You’re overwhelmed but still engaged. You care about what you’re doing, you’re just running low on resources. Most stress management strategies work well here.
Stage 2: Overextension. The warning signs start showing. Persistent fatigue, cynicism creeping in, performance starting to slip. You’re still functioning, but something’s off.
Stage 3: Burnout. Emotional numbness. A deep sense of detachment from your work or responsibilities. Inability to feel satisfaction even when things go well. Physical exhaustion that sleep doesn’t fix. This is where self-care strategies alone stop being enough.
Key burnout symptoms to recognize:
- Feeling emotionally numb or disconnected from things that used to matter
- Cynicism or resentment toward people or work you once cared about
- A persistent feeling that nothing you do makes a difference
- Exhaustion that remains regardless of how much you sleep
- Dreading every single day before it starts
One of the most important things to understand about burnout: the stressor source has to change. You can practice all the self-care in the world, but if the conditions driving the burnout stay the same, recovery will be temporary at best.
Our guide on preventing burnout before it starts walks you through the early warning signs and what to do about them.
Long-Term Stress Management: Building a Daily Routine That Sticks
Quick-fix techniques are valuable. They help you get through a hard moment. But genuine, lasting stress resilience comes from something different: consistent daily habits that keep your nervous system regulated before the crisis hits.
Think of it this way. Every decision you have to make uses a small amount of mental energy. By the end of the day, that energy is depleted. Stress makes decisions feel harder, which depletes your resources faster, which makes the next stressor worse. A routine cuts through this. When you don’t have to decide how to start your morning or wind down your evening, those choices are already made. Your brain gets to rest.
Here’s a simple framework to build from:
Morning Anchor (20–30 minutes total)
- Consistent wake time. Same time every day, weekends included. This is the single highest-impact sleep and stress habit.
- 5 minutes of movement or breathwork. It doesn’t have to be a workout. A short stretching sequence or box breathing session is enough to lower morning cortisol.
- A protein-rich breakfast. Blood sugar stability in the morning significantly reduces stress reactivity through the rest of the day.
Daytime Buffers
- Two scheduled micro-breaks. Even a 5-minute walk away from your desk lowers cortisol and improves focus. Set a timer if you have to.
- Limit caffeine after noon. Caffeine has a half-life of 5–6 hours in most people. An afternoon coffee is still affecting your cortisol at 10pm.
- Some nature exposure if possible. Even 10 minutes outside in natural light shifts your nervous system in measurable ways.
Evening Wind-Down (30–45 minutes before bed)
- Turn off the screens 30 minutes before sleep. Non-negotiable for cortisol regulation.
- Brief journaling or a gratitude note. Three things that went well today. Sounds small. The research on its cumulative effect is not.
- The same bedtime. Your body clock rewards consistency far more than duration.
When I started building a morning anchor about 18 months ago, I didn’t feel different on day one. By week three, though, the ritual had become automatic. And with that automaticity came something I hadn’t expected: a genuine buffer between me and the first stressor of the day. That gap, even just a few seconds of it, changes how you respond.
For more on building habits that last, our guide to daily stress-reducing habits gives you the full framework. And if your body’s already showing signs that it’s running on empty, read our post on when your body needs a break first.
When Should You Seek Professional Help for Stress?
You should seek professional help for stress when it persists for more than a few weeks, interferes with work or relationships, causes physical symptoms like chest pain or persistent insomnia, or leads to feelings of hopelessness or thoughts of self-harm. Despite 63% of Gen Z rating their mental health as “less than good,” only 1 in 4 adults sought professional support in 2024.
Let’s address something directly: getting professional help for stress is not a last resort. It’s not something you do when everything else has failed. It’s a tool, just like exercise or sleep hygiene, and for many people it’s the most effective one.
The APA’s 2024 data shows that only 24% of adults spoke to a mental health professional in the past year, despite the majority reporting significant stress levels. That gap between needing support and seeking it is worth closing.
Three therapy approaches are particularly well-supported by research for stress:
Cognitive Behavioral Therapy (CBT) is the most researched. It works by identifying the thought patterns that amplify your stress response and replacing them with more accurate, balanced ones. Most people see meaningful results within 8–12 sessions.
Mindfulness-Based Cognitive Therapy (MBCT) combines meditation with CBT techniques. It’s particularly effective for people who experience anxiety alongside stress, or who have a pattern of recurring low mood.
Brief Solution-Focused Therapy is shorter-term and practical. Rather than exploring root causes at length, it focuses on what’s working and how to build on it. Good for people dealing with a specific, identifiable source of stress.
The National Institute of Mental Health confirms that spotting stress symptoms early, and getting support quickly, prevents long-term anxiety, depression, and burnout from developing. Waiting until you’ve hit a wall is not necessary and often makes recovery longer.
See a doctor or mental health professional if:
- Your stress has lasted more than 2–3 weeks without improving
- It’s affecting your relationships, your work performance, or your physical health
- You’re using alcohol, drugs, or other behaviors to cope
- You’re experiencing persistent feelings of hopelessness or thoughts of harming yourself
Our guide to how therapy helps with stress explains your options in plain terms. And if you’re wondering about structured outpatient support, our post on outpatient mental health options covers what that actually looks like day to day.
Your Complete Stress Management Resource Directory
Want to go deeper on any of the topics above? Every section of this guide has a dedicated post with full details, specific techniques, and sources. Here’s where to go next:
Understanding and recognizing stress. Read our full breakdown of the emotional signs of stress and what chronic stress does to your body over time.
Fast and natural stress relief. Our roundup of more quick stress relief techniques gives you 10 methods you can start using immediately.
Stress and sleep. If your brain won’t stop at night, read why stress keeps your brain awake and what to do about it.
Food, diet, and stress. Learn how to build a daily diet that supports your stress response with our guide to greens that support stress relief.
Exercise and movement. Start with our stress-relieving home workouts — no gym required.
Teen and family stress. Parents, read our guides on stress signs in teenagers and helping your teen cope with pressure.
Burnout recognition and recovery. Start with our guide to preventing burnout before it starts.
Therapy and professional support. Read how therapy helps with stress and explore outpatient mental health options if you’re ready for more structured support.
Putting It All Together
Stress is not a character flaw. It’s not a sign that you’re weak or that you’re failing at life. It’s a physiological response that every human being has, and it can be worked with.
Three things to take from this guide:
First, your body gives you signals before stress becomes a crisis. The headaches, the poor sleep, the short temper. These aren’t inconveniences. Their information. Pay attention to them early.
Second, small, consistent habits are what build lasting stress resilience. Not one dramatic weekend retreat. Not a single perfect meditation session. Just a morning anchor, a wind-down routine, some movement, and decent food. Repeated. Over time.
Third, getting help is not a last resort. Whether that’s a therapist, a doctor, or just a conversation with someone you trust, reaching out early makes every other strategy work better.
Start wherever the need is greatest right now. You don’t have to overhaul everything at once.
What’s your biggest stress trigger right now? Drop it in the comments below. We read everyone.
Disclaimer: This guide is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. If you are experiencing severe stress, mental health difficulties, or thoughts of self-harm, please seek support from a qualified healthcare professional.
Last reviewed: April 2026
Frequently Asked Questions
What is the most effective stress management technique?
The most effective stress management technique varies by person, but mindfulness meditation has the strongest research base. Harvard Medical School research shows consistent practice can reduce cortisol by up to 25% over 8 weeks. In practice, combining techniques works better than relying on any single one. Pairing daily breathwork with regular exercise and consistent sleep habits tends to produce the most lasting results.
How does stress affect the body physically?
Stress triggers the release of cortisol and adrenaline, raising heart rate and blood pressure and tensing the muscles. Over time, chronic stress suppresses the immune system, disrupts digestion, increases the risk of heart disease and high blood pressure, and contributes to weight gain. The National Institute of Mental Health confirms that untreated stress can lead to serious long-term health conditions, including anxiety disorders and depression.
How long does it take for stress management techniques to work?
It depends on the technique. Quick methods like box breathing and the 5-4-3-2-1 grounding exercise lower cortisol and heart rate within minutes. Consistent habits like exercise and improved sleep take 2–4 weeks to produce sustained cortisol reduction. Harvard Medical School research shows that a daily mindfulness practice produces measurable changes in the brain’s stress response after approximately 8 weeks of consistent practice.
Can stress cause physical illness?
Yes. The APA’s research shows that chronic stress is directly linked to heart disease, high blood pressure, weakened immunity, digestive disorders, and increased risk of anxiety and depression. It can trigger or worsen skin conditions like eczema and psoriasis, cause persistent headaches, and disrupt hormonal balance. The physical effects of chronic stress are not minor. They are among the leading contributors to poor health outcomes in adults.
What is the difference between stress and anxiety?
Stress usually has an identifiable external cause: a deadline, a difficult relationship, or financial pressure. When the trigger resolves, the stress typically eases. Anxiety often persists without a clear cause and can feel like a constant background hum of worry or dread. Both involve the same cortisol and fight-or-flight response, but anxiety disorders are clinical conditions that typically require professional treatment rather than lifestyle changes alone.
What foods help reduce stress?
The best foods for lowering stress include magnesium-rich options like dark leafy greens, pumpkin seeds, and dark chocolate (70%+), omega-3 fatty acids from salmon and walnuts, and probiotic-rich foods like yogurt and kefir that support gut-brain communication. Research shows that even mild dehydration raises cortisol levels, so staying hydrated is also important. Avoid caffeine after noon and limit alcohol, which disrupts sleep and worsens next-day anxiety.
How does exercise help with stress relief?
Exercise lowers cortisol and triggers the release of endorphins, the brain’s natural mood stabilizers. The APA recommends at least 150 minutes of moderate physical activity per week for mental health benefits. Even a 20-minute walk measurably reduces cortisol levels within the hour. The key is consistency at moderate intensity. Excessive high-intensity exercise every day can actually spike cortisol rather than lower it.
When should I see a doctor about stress?
See a doctor or mental health professional when stress persists for more than 2–3 weeks, starts affecting your work, relationships, or physical health, or leads to chest pain, persistent insomnia, or feelings of hopelessness. The APA’s 2024 data shows only 24% of adults sought professional mental health support in the past year, despite the majority experiencing significant stress. Getting help early, not as a last resort, leads to faster and more complete recovery.
About The Author:
Christy Houston, LMSW, LCSW – Psychotherapist
Been in practice 10+ years. Christy also works in the Beaumont Health Care System in the Mental Health Department, which includes Partial Hospital Program, 3MHU, & social work consults in the Emergency Dept.
Degrees & Certifications
Licensed Master Social Worker in the State of Michigan
She received a Master of Social Work from Wayne State University, majoring in Mental Health
