Living with Type 2 Diabetes can be difficult, even more-so when combining it with obesity.
Deemed as a silent killer, it can increase the risk of heart disease, kidney disease, vision problems, and other diseases and common comorbidities.
Weight loss in obese individuals has been seen to have a positive effect on the decrease of negative outcomes related to the disease.
As such, doctors encourage lifestyle and diet changes, and even behavioral modification techniques, to help minimize the long-term effect of Type 2 Diabetes on the body.
However, it’s important to note that these are not the only options available to individuals with the disease.
While modifications to diet and the addition of exercise is the first step, this is a slow option that may sometimes not be appropriate for the patient’s health outcomes.
Diabetes surgery has had many technological advancements that have seen the rise in options for safe interventions for individuals, and its effects are long-lasting due to the procedures.
As such, when coupled with healthy habits and physical interventions, bariatric surgery can help diabetes patients get back on track with their health goals.
The Risk Factors of Type 2 Diabetes
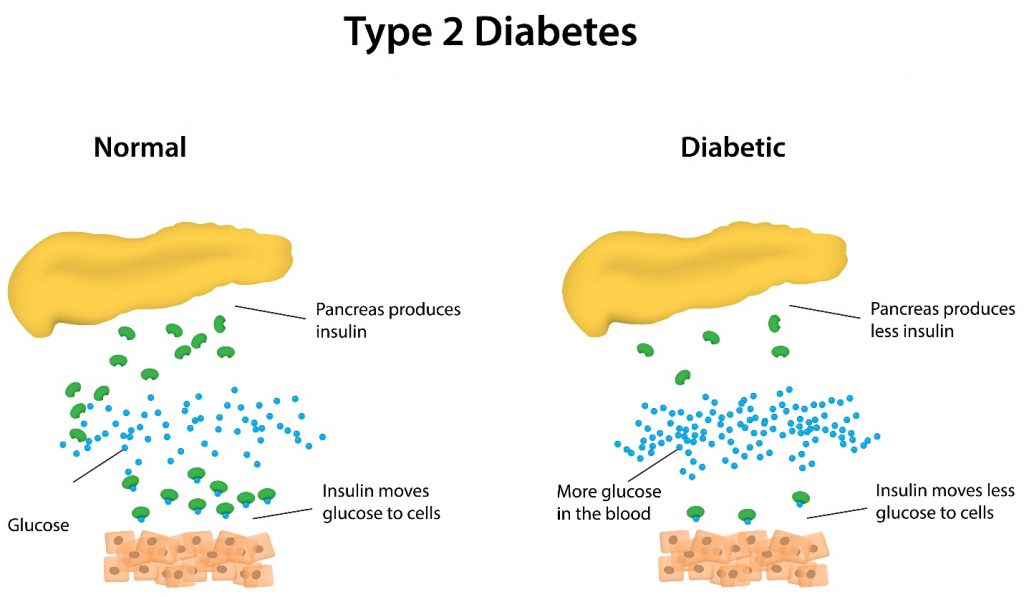
It is important to note that there are two types of diabetes. Type 1 diabetes refers to the condition in which a minimal amount, or no insulin, is produced by the pancreas, which then affects cell energy as it restrains the glucose from entering the cells of the body.
This type of diabetes is thought to be caused by environmental factors as well as a family history of this particular type of diabetes.
Type 2 diabetes, on the other hand, is closely related to obesity, which is when an individual has excess body fat that adversely affects their health.
This is determined by an individual’s Body Mass Index (BMI), which is used to assess what a specific patient’s appropriate body weight should be by taking into account their age, sex, and height.
Obesity heightens the risk of type 2 diabetes as this condition indicates a progressive resistance to the effects of insulin produced in the body, as well as the gradual loss of insulin production as needed by the body to function.
Type 2 diabetes is typically seen in individuals aged 45 and above.
Ascribing to healthy lifestyle habits such as regular exercise and proper diet has been seen to have an effect on reducing the risk factors for developing diabetes.
However, if diagnosed late, this may not be enough to combat both weight issues and the issues that can arise from diabetes that have been left unchecked for a significant period of time.
In Perth, bariatric surgery should be considered in individuals with a BMI greater than 35, and who have not seen significant results with medication and lifestyle changes, or in individuals who have a BMI of 30 to 34.9 and have other underlying health conditions that can be aggravated by lack of intervention.
Bariatric Surgery As An Intervention
When diagnosed with type 2 diabetes, doctors recommend lifestyle changes. In some individuals, the caloric intake is not offset by exercise, the body weight increases, and with it, risk factors for serious diseases.
To combat this, doctors are known to work with patients to encourage healthy eating and regular exercise, and maybe even look into behavioral modification techniques to influence their patient’s relationship with food.
As this can have a significant role to play in unhealthy eating habits. This is aside from prescribing medication to help with glucose levels to attempt to return the body to a normal state of function.
However, it is important to note that while this is the standard intervention for diagnosis, it is not the only intervention available.
For individuals who require significant weight loss or those who have not seen enough positive results following dietary modification and exercise coupled with medication, diabetes surgery should be considered.
If you’re in Perth, bariatric surgery is done via laparoscopy, which is a minimally invasive method.
Gastric Restrictive Procedures
It limits caloric intake by providing a feeling of fullness or satiety, encouraging weight loss. Studies have shown that after undergoing the procedure, patients lose around 10 to 20% of their body weight.
These types of procedures are done by means of making small incisions and restricting the area of the stomach so that a limited amount of food intake will be enough for the patient to feel full.
It is important to note that this type of surgery results in weight loss, as well as influences insulin sensitivity, and patients who have undergone the procedure have seen a remission in their type 2 diabetes.
Intestinal Bypass Procedures
It is a permanent intervention and reduces caloric intake by means of shortening the area of the small intestine.
With less of the small intestine being used by the body, there is reduced absorption, which has positively affected most patients who have undergone the procedure leading to type 2 diabetes remission.
For individuals who have had diabetes for a longer period of time and have exhausted lifestyle changes and medications with minimal effect, this may be a better option to ensure weight loss outcomes and reduction of risk factors as influenced by untreated diabetes.
Final Thoughts
Individuals suffering from obesity and diabetes, and who have not seen significant results with the standard interventions would do well to consult with their doctor for a reputable Perth bariatric surgeon.
When taking the individual’s specific age, lifestyle changes, and possible recovery time into consideration, diabetes surgery is a safe option for those suffering from the condition, and who need to see a significant change to ensure their quality of life.
About The Author:
Dr. Andrew Kiyingi is one of Perth’s premier Specialist Weight-Loss Surgeons. With over 16 years of clinical experience both locally and globally he is an accredited Surgical Trainer with the Royal Australasian College of Surgeons.
After completing surgical training at St Vincent’s Hospital in the early stages of his career, Dr. Kiyingi was awarded Fellowship under the Royal Australian College of Surgeons (FRACS). In 2016 he was further awarded the Phoenix Health Bariatric Fellowship in Liverpool.




